research and projects
Find out our projects

Research and fund-raising
From 1993 to the present the research sustained with significant sums by authorative laboratories and outstanding care institutions has allowed us to get to more and more satisfactory results in terms of quality of life and long-term survival of young patients.
Genedren (Gen-children)
Neuroblastoma has a distintive trait which differentiates it from adult cancer. Since it’s onset occurs very early during development, in some rare cases even in uterus, cells that produce it have had little time to develop and accumulate mutations. This knowledge comes from the possibility of analysing the entire genome sequence. Neuroblastoma is known as the tumor with the least mutated genome ever. It is therefore evident that children affected by Neuroblastoma are genetically predisposed to develop the disease and therefore carry risk mutations inherited from their parents. The GENEDREN project aims to identify these alterations, incrase knowledge about the development of Neuroblastoma and transfer them to clinic. The project can be realized in three to five years and requires to be done a total investment of 1,152,000 euros, of which 791,000 are borne by the FNb and 361,000 by co-financing of other organisations.
IMMUNB (Immunotherapy for Neuroblastoma)
The goal is the development of a new, innovative and promising immunotherapy approach for patients with high-risk to develop Neuroblastoma (NB). To date, only immunotherapy based on the use of ant-GD2 antibody (indicates the drug produced by “dinutuximab”) that recognizes GD2 protein expressed on the surface of NB cells, is used in the United States and Europe for patiens with high-risk NB. In this context, one should keep in mind that a cellular protein, in order to be considered a target that can “strike” safely, should be abundantly expressed by cancer cells but it shouldn’t be on healthy cells. These traits have been identified in the B7-H3 protein, which becomes again a new potential immunotherapy target for NB. With these premises I twill be possible to develop an innovative treatment, already effective in several adult tumour models: the aim is to verify if also on pediatric tumors, particulary on NB same results can be obtained. If the already existing studies will confirm it we can move on to clinical trials on young patients to improve prognosis in patients affected by NB, relapsing or refractory to chemotherapy.
Pensiero Project:
“Histological Centralization, Biobanks and Registry
of Central Nervous System Pediatric Tumors”.
“Pensiero Project” was born in 2008 from the need to offer the scientific community information and tools to reduce diagnostic discrepancies as to say those that determine a change in therapy for the young patient.
The percentage of such discrepancies has decreased from an initial 35% to today’s 0.1%.
This has been possible thanks to the histopathological centralization of pediatric Central Nervous System (CNS) tumor cases. The synergy and collaboration between treatment centers of excellence such as Bambino Gesù Hospital in Rome, Santobono Hospital in Naples, Meyer Hospital in Florence, Bellaria Hospital, City of Science and Health in Turin, Gaslini Institute in Genoa, Besta Hospital in Milan and others coordinated by dr. Giangaspero from the University La Sapienza of Rome has allowed the drafting and expansion of CNS registry of tumors, as well as updating the “virtual” biological bank that represents about 32,5%(884/2723) of centralized cases of which we have biological material available for basic and translational studies.
An average of approximately 240 new cases are enrolled each year.
Clinical and Biological Activity
Project for the coordination of clinical and
experimental research in Italy.
Neuroslatoma (NB) is the most frequent extracranial solid tumor of pediatric age (8-10% of all tumors in the age group 0-16 years) with about 130 diagnosed cases every year in Italy.
Since 1976, researchers from Giannina Gaslini Institute have been coordinating, within AIEOP, what is currently called as the “Neuroblastoma Working Group” (GdLNB), which has the task of activating national and international therapy protocols and planning scientific research about this neoplasm.
Institute Gaslini in 1994 was one of the 4 founding centers of the European Cooperative Group, which today can count 26 member states. In 2016 it was recognized by Liguria region as a reference center for Neuroblastoma and in 2017 it was included among the European reference centers within the Paediatric Cancer European Reference Network (PaedCan ERN).
Context
Neuroslatoma (NB) is the most frequent extracranial solid tumor of pediatric age (8-10% of all tumors in the age group 0-16 years) with about 130 diagnosed cases every year in Italy. Since 1976, researchers from Giannina Gaslini Institute have been coordinating, within AIEOP, what is currently called as the “Neuroblastoma Working Group” (GdLNB), which has the task of activating national and international therapy protocols and planning scientific research about this neoplasm. Institute Gaslini in 1994 was one of the 4 founding centers of the European Cooperative Group, which today can count 26 member states. In 2016 it was recognized by Liguria region as a reference center for Neuroblastoma and in 2017 it was included among the European reference centers within the Paediatric Cancer European Reference Network (PaedCan ERN).General Aims
In the last 30 years thanks to a centralization project of young patient data, it has been possible compile the NB registry with 4120 patients. It is essential to have information and tools that can allow to formulate a timely and accurate diagnosi as well as to define treatment protocols targeted to young patients. This is the result of an diligent multidisciplinary work between different specializations, among which we can mention: The Italian Register Neuroblastoma active since 1979 prospectively collects informations about all the Italian patients affected by NB and treated within AIEOP centers. To date, RINB can count over 4000 cases, resulting in an avergae annual enrollment of approximately 120 new cases. Since 2016, RINB has resided on a secure, web accessible information technology platform by all centers collaborating with it. The service of centralization and analysis of tumor tissue and other biological materials. Thanks to this service (commonly defined using the term Biocase, which represents the method by which materials are sent from peripheral centers to Gaslini) all children with NB are guaranteed an adequate histopathological, biochemical and genetic characterization of the tumor at the onset as well as during the follow-up. The Integrated Biobank Tissue Genomics-BIT Gaslini, started in 2009, collects materials centralized by AIEOP centers as well as materials from other European institutes. It processes and catalogs tumors as well as processing a molecular databse available to researchers on which therapeutic protocols are designed.Our goals for 2022-2024:
- Continue to ensure a high and homogeneous quality in clinical, histological and biological classification as well for what concerns the treatment of children with Neuroblastoma referred to Italian Oncology Centers(AIEOP).
- Guarantee material and data to explore the meaning in biological and prognostic terms of studied bio-molecular features and to support a highest interchange between basic and clinical biology.
- Develop advanced and translational research lines.
The Lab
Foundation’s laboratory began to be an independent reality dedicated to research on Neuroblastoma and Pediatric Solid Tumors in 1994. The Laboratory is equipped with innovative technology and spaces to host scholars from abroad, news students and young graduates to be trained for the future of Research. During these years the lab has become a reference point for reseach that interacts with the most qualified international research centers in different fields like:diagnostics,genomics,transcriptomics,embryology applied to disease, new nanotechnologies and recently development of experimental therapeutic protocols. Today we use the term “NB-LABnetwork” to refer to the network of laboratories of excellence that work together united to advance Neuroblastoma Research NB-LABnetwork: The National Network of Laboratories was created to facilitate the advancement of translational research by creating strategic synergies that permits to speed up results achievements. The NB-LABnetwork connects, highlights and makes competences, advanced technological platforms and research programs of Italian groups easily recognizable. The Italian groups we are talking about have been engaged in the fight against Neuroblastoma for years. The NB-LABnetwork also aims to promote the training of young researchers by supporting university PhD programs, research grants, masters and training courses.
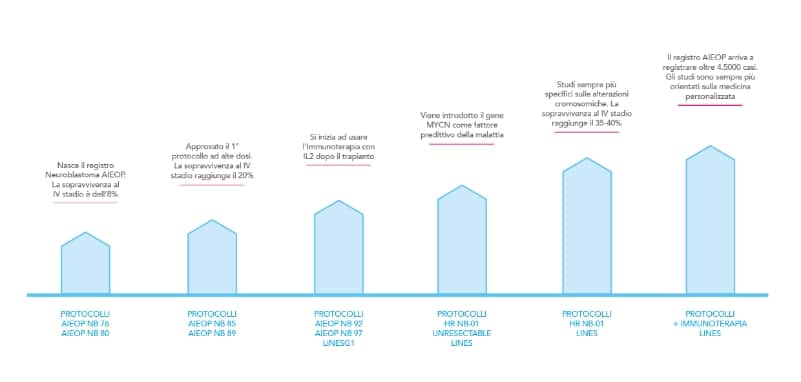
The Arrow of Hope
In the last 30 years, thanks to the research supported by our Association, important steps forward have been made both in terms of long survival of young patients as well of increasingly personalized treatment protocols.
Here is a summary of the main steps achieved so far in this long journey of hope:
Lab goals:
Since 1994 the Laboratory has been at the forefront for the most advanced researches on Neuroblastoma. Researchers use high-level technologies (Next Generation Sequencing –NGS for example) for increasingly and detailed genomic analysis.
Here are the key milestones achieved:
-
1994
Creation of ENQUA Group:
a European group for the quality control of molecular biology data. The laboratory is appointed to the italian referent. -
1995
All italian cases of neuroblastoma(NB) are analyzed for MYcN and LP36 using FISH technique. The laboratory is the National Reference for these examinations.
-
1996
CGH in metaphasics: for the first time in Italy, analysis of comparative Genomic hybridization metaphasica on NB samples is performed at the laboratory.
-
1997
The phenomenon of apoptosis in NB cells is studied.
-
1998
At the laboratory and in collaboration with S.C. genetics of STI tumors a new variant of splicing of p73 /p73A/ in NB is identified.
-
1999
“NB family: at the laboratory a new study about family NB begins. The study is aim to identify genes associated with NB development.
LNESG1: closes the first European protocol on localized NB in which the laboratory participated as an Italian referent. -
2000
Spotter Array: is purchased by NB Foundation one of the first spotters present in Liguria for the preparation of microarray.
The laboratory partecipates in tumors analysis in European protocol INFANTS for NB treatment. -
2001
ArrayCGH: For the first time in Italy at the laboratory the analysis of NB cells genome by means of high-density microarrays is performed.
The laboratory participates in tumors analysis of the European protocol UNRESECTABLE for NB treatment. -
2002
Study of the expression of p73A as a molecular marker of NB.
-
2003
Gene Expression Profiling: For the first time in Italy at the laboratory analysis of gene expression of NB cells by means of Microarrays are performed and new “gene signatures” of Nb are identified.
-
2004
ANR in Genoa: researchers of the laboratory partecipate with several communications at the International Congress Advanced NB Research organized by NB Foundation.
-
2005
Microdissection: For the first time in Italy at the laboratory a microdissection of tumor tissue of NB by means of a laser beam has been performed. The selected cells DNA will be analyzed with arrayCGH. At the laboratory the study of brain tumors genomics has started with particular regard to Medullcblastcma.
-
2006
In the laboratory, genome of neural crest cells is studied during embryonic development of the mouse.
Tissue microdissection and gene Expression Profiling: experiments are repeated to isolate cancer cells by means of laser microdissection. On such cells, genetic expression is studied by means of Microarrays. -
2007
MLPA: in accordance with european protocols, the laboratory performs pangenomic examination on NB cells by means of Multiplex Ugation-dependen Probe Amplification.
-
2008
ALK: from the study of family NB we come to the discovery of ALK (the first gene associated with NB predisposition.
-
2009
ALK as a pharmacological target. Start of ALK inhibitors for the development of therapeutic protocols.
The first experiment of miRNA analysis regarding expression profiles by means of Microarrays in NB samples is performed. -
2010
Analysis of Neuroblastoma genome by means of Next Generation Sequencing has began. This is a cutting-edge technology to analyze in better detail mutations associated with tumor development.
-
2011
2 ALK inhibitors are being studied in vitro and in vivo experimental models.
-
2012
A medicobiological working group was established to evaluate the launch of a pilot protocol with an ALK inhibitor.
The next generation sequencing analysis of tumors for patients with high-risk NB was performed. The study involves the search for those genes that can make the tumor aggressive and treatment-resistant. -
2013
Opening of the new laboratory on Neuroblastoma based at IRP (Pediatric Reserarch Institute) in Padua.
Start-up of laboratory and new research team. Projects on ALK inhibitor and genome analysis of high-risk neuroHastoma are being pursued. -
2014
The team now includes 6 researchers.
An important agreement with Ignyta (USA pharmacological company) for study a new ALK inhibitor is signed. The next generation Sequencing analysis identified several genes associated with high-risk NB. -
2015
Study on chomosome instability (CIN) in Neuroblastoma.
-
2016
Production of new preclinical models for the study of pharmacological activities for applicable treatments to Neuroblastoma therapy.
-
2017
Outcome results of the study about exoma mutation in high risk-patients tumors.
-
2018
The role of Lin28b gene for the development of Neuroblastoma in predinal studies and in metastic disease is confirmed.
-
2019
A new 3D model has been realized in vitro to study the biology of metastatic cancer in bone marrow microenvironment.
“Single celi” genomic analysis techniques will be used in future to identify metastatic activity of Neuroblastoma.
Follow up studies on autophagy in preclinics.
From 1979 to 1986: Neuroblastoma registry AIEOP is born. Survival at the fourth stage is 8%.
PROTOCOLS: AIEOP NB 76, AIEOP NB 80
From 1985 to 1992: The first high-dose protocol is approved. Survival rate at the fourth stage reaches 20%. AIEOP NB 85, AIEOP NB89
From 1992 to 1998: Immunotherapy with IL2 is started after transplantation. AIEOPNB92, AIEOP NB97, LINESG 1
From 1999 to 2005: MYC-N gene is introduced as a predictive factor of the disease. HR NB-01 UNRESECTABLE LINES
From 2006 to 2011: Increasingly specific studies on chromosomal alterations. Survival at the fourth stage reaches 34-40%. HR NB-01 LINES
From 2012 to 2019: AIEOP registry records over 4.500 cases. Studies are increasingly oriented towards personalized medicine.
HR NB-01 + IMMUNOTHERAPY LINES